Allergic Diseases
A Guide from Symptoms to a Full Life
We provide complete care for allergies of the airways, skin, food, and insect venom. Our goal is to bring your symptoms under control and give you back the comfort of everyday life.

Allergic Rhinitis and Conjunctivitis

Allergic rhinitis is an unpleasant but very common condition in which the immune system overreacts to substances in the environment, known as allergens. Typical allergens include pollen, house dust mites, moulds, animal dander, and certain occupational substances. Allergic rhinitis is often accompanied by conjunctivitis, which affects the eyes. The two conditions usually appear together, flare up at the same time, and share the same causes.
Symptoms That Should Bring You to a Doctor
- sneezing, itching in the nose, a blocked nose, or a watery runny nose
- itchy and watering eyes, redness of the conjunctiva, swollen eyelids
- fatigue and disturbed sleep caused by a blocked nose
- symptoms that worsen on contact with a trigger (for example in spring or after contact with a cat)
- symptoms lasting more than a week without fever or muscle pain
How the Condition Is Diagnosed
The doctor first asks in detail about your symptoms, how they have changed over time, and any possible context (season, pets at home, occupation). Specialist tests then follow: skin prick tests, blood tests for specific IgE antibodies, and component-resolved diagnostics, which helps distinguish a true allergy from simple sensitisation. In some cases we add an examination of the nasal lining or the conjunctiva.
Treatment Options
- avoiding allergens (window filters, washing bedding, limiting contact with animals)
- medication (antihistamines, corticosteroid nasal sprays, eye drops)
- allergen immunotherapy, the only treatment that can address the underlying cause of the allergy
What You Can Do at Home
- follow the pollen forecast, available online and in mobile apps
- air rooms briefly and in the morning (when pollen levels are lower) and wear sunglasses outdoors
- wash your face, hands, and hair after coming in from outside
- wash bedding regularly and use anti-mite covers
When to Book an Appointment
- if your symptoms last longer than a week
- if the problem comes back regularly (for example every spring)
- if standard over the counter medication is not enough
Bronchial Asthma

Bronchial asthma is a chronic inflammatory disease of the airways, marked by their increased sensitivity and by variable, usually reversible narrowing. This can lead to repeated episodes of breathlessness, coughing, and wheezing. Asthma is often linked to allergy (for example to pollen, mites, or animal allergens), but it can also be triggered by infections, physical exertion, cold air, irritants, or stress.
Symptoms That Should Bring You to a Doctor
- repeated breathlessness, a sense of not getting enough air, or chest tightness
- wheezing or whistling sounds when breathing
- a long-lasting, often dry cough (especially at night or in the early morning)
- worsening symptoms during exercise, in cold air, or on contact with a trigger
- waking at night because of coughing or breathlessness
- feeling restricted in everyday activities
- repeated bouts of “bronchitis” with no clear cause
How the Condition Is Diagnosed
The doctor focuses on the character of your symptoms, how they vary over time, and possible triggers. The basic test is spirometry, which assesses lung function and airway flow. It is often supplemented by a bronchodilator reversibility test (to confirm whether the airway narrowing reverses with medication), and where appropriate by fractional exhaled nitric oxide (FeNO), which reflects the level of airway inflammation. Allergy testing is usually part of the workup as well.
Treatment Options
- inhaled corticosteroids (the foundation of treatment, calming inflammation in the airways) and bronchodilators, including combination inhalers
- treatment of the underlying allergy (including allergen immunotherapy in suitable patients)
- lifestyle measures and trigger control
What You Can Do at Home
- use your prescribed inhaled medication regularly, even when you feel well
- learn the correct inhaler technique
- avoid known triggers
- do not smoke and stay out of smoky environments
- keep up regular, moderate physical activity
Skin Allergies
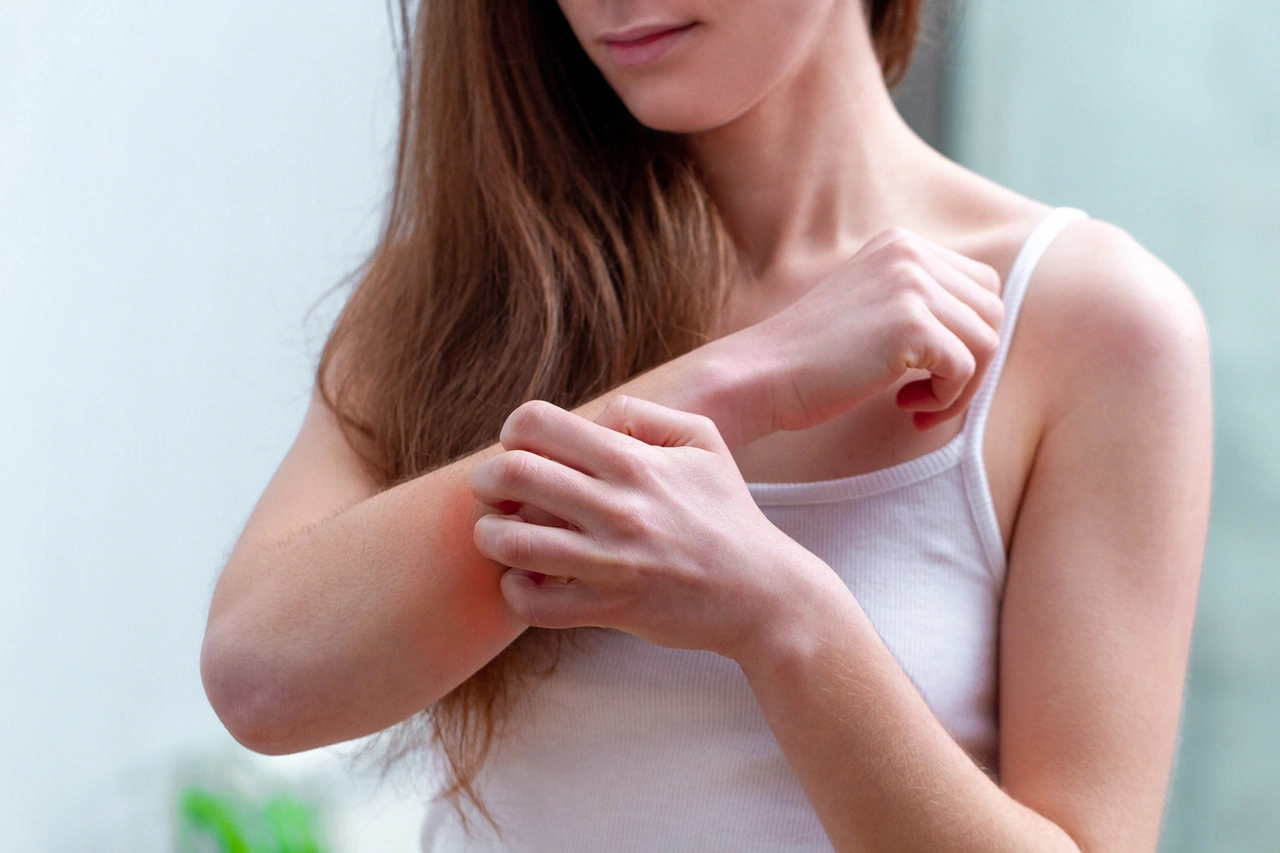
Urticaria
Urticaria is a skin condition marked by an outbreak of itchy, fleeting wheals. It can also appear as red patches on the skin or as swelling of the skin, the deeper tissues, or the mucous membranes. A short-term episode may be linked to an allergy to medication, food, insect venom, or airborne allergens. A long-lasting form can be triggered by physical stimuli (cold, heat, sun exposure, friction, physical exertion), or it may have no external trigger at all (chronic spontaneous urticaria, formerly called idiopathic urticaria).
Treatment
- antihistamines (oral allergy tablets), at higher doses in more severe cases; short courses of corticosteroids when there is swelling; the most severe cases are managed in specialist centres.
Atopic Eczema
Atopic eczema (also called atopic dermatitis) is a chronic, non-infectious inflammatory disease of the skin that often lasts for many years and sometimes a lifetime. The typical changes most often appear in childhood; in some patients they continue into adulthood, and less often the condition appears for the first time in adulthood. It develops through a combination of genetic factors and influences from the outside environment (airborne allergens, food, irritants) and the internal environment (hormones, infection, the gut microbiome, an overreactive immune system). A central factor leading to dry, more permeable skin is a breakdown of the skin’s protective barrier function (water is lost, sebum production drops, and chemicals and allergens pass more easily into the skin).
Symptoms That Should Bring You to a Doctor
- redness and itching of the skin, poor sleep, irritation, rashes, dryness, scaling, weeping, and crusting
- the suspicion that food or environmental allergens are triggering or worsening the condition
- the presence of other allergic conditions (hay fever, perennial rhinitis, bronchial asthma)
How the Condition Is Diagnosed
The diagnosis should be made by a dermatologist on the basis of the clinical findings. The allergist contributes by identifying possible triggers and aggravating factors, namely the allergens that influence the course of the disease, through blood tests for specific allergic antibodies or skin testing with allergens. The allergist can also diagnose other allergic conditions that may appear later in life, such as allergic rhinitis or allergic bronchial asthma. This sequence is known as the atopic march.
Treatment Options
The foundation is topical treatment, ideally led by a dermatologist. Constant, regular moisturising of the skin with products called emollients is essential. Emollients hydrate the skin, restore its protective film, and improve elasticity. Where needed, the dermatologist or allergist will add topical products with anti-inflammatory or immunomodulatory effects. When allergens are confirmed to play a role, topical care is supplemented by systemic antihistamines. In the most severe forms of atopic eczema, the allergist works with the dermatologist to introduce immunosuppressive or biologic therapy. If the skin becomes infected, antibiotics are needed.
In early childhood, where food allergens are a frequent trigger (most often cow’s milk protein and egg), an elimination diet or a special diet (amino acid based formulas) has clear therapeutic value.
What You Can Do at Home
- Moisturise the skin regularly, even when no active patches are present.
- Use gentle, non-irritating cosmetic products designed for eczema-prone skin.
- Avoid long baths in hot or chlorinated water.
- Prevent overheating and choose suitable clothing (cotton).
- Limit skin contact with chemicals and solvents.
- During flares, cut back on irritating foods (citrus fruit, sour or fermented foods, chocolate, spicy dishes), do not smoke, do not drink alcohol, and avoid any food to which an allergy has been confirmed.
- Limit contact with confirmed allergens.
- Spend time outdoors regularly; spa and seaside stays can be beneficial.
- Keep stress under control
When to Book an Appointment
Especially when there is a suspicion that flares are driven by food or inhaled allergens. When other allergic symptoms are present, such as a runny nose, itchy eyes, cough, or breathlessness.
Insect Sting Allergy (Bee, Wasp, Hornet)

An allergy to the venom of Hymenoptera insects is caused by an excessive immune reaction to the venom delivered by a sting. Two scenarios occur: a large local reaction, or a severe allergic reaction that can progress to anaphylactic shock.
Large Local Reaction
This shows up as swelling that is greater than usual (for example, after a sting on the elbow the whole arm swells). Cool the site of the sting, take an antihistamine (Zyrtec, Zodac, Claritine, or Xyzal) and a corticosteroid (prednisone). Keep these medicines on hand from your doctor. With less pronounced swelling, the prednisone tablet can be replaced by a corticosteroid ointment. Continue treatment for several more days.
Severe Allergic Reaction: Anaphylactic Shock
Symptoms include difficulty breathing, chest tightness, hives, restlessness, a fast pulse, nausea, and disturbed consciousness. Not all of them have to appear at once. The reaction can develop very fast and lead to cardiac arrest.
WARNING: First Aid for Anaphylaxis (a Life-Threatening Reaction)
Symptoms include difficulty breathing, chest tightness, hives, restlessness, a fast pulse, nausea, and disturbed consciousness. Not all of them have to appear at once. The reaction can develop very fast and lead to cardiac arrest.
Call 155 (the Czech emergency number) immediately
and report an “anaphylactic reaction.”
Use the adrenaline auto-injector (EpiPen)
into the outer thigh (even through clothing)
Give an antihistamine and a corticosteroid
Only then administer an antihistamine and a corticosteroid, and only if the patient is conscious.
Lie the person flat with the legs raised
Ensure the patient is positioned appropriately, preferably lying down with the lower limbs elevated, monitor vital signs, and initiate resuscitation if necessary.
When emergency services arrive, report the medications administered and the course of the reaction, and hand over the used epinephrine auto-injector.
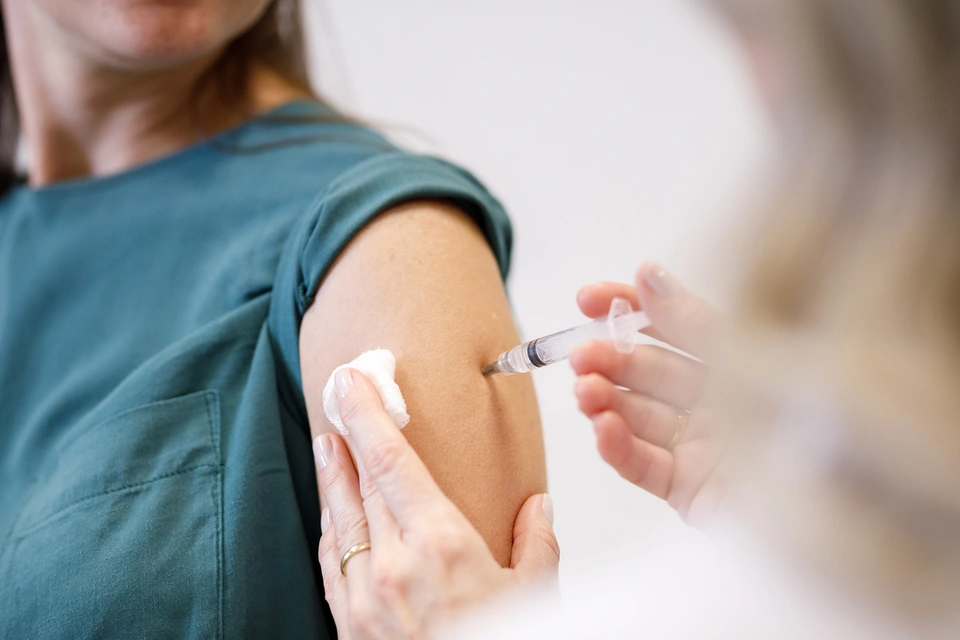
Allergen Immunotherapy for Hymenoptera Venom Allergy
This is a targeted treatment in which a small, gradually increasing dose of the allergen is given to the patient, allowing the body to become accustomed to it. The vaccine is given by injection; once the maintenance dose is reached, the interval is roughly four to six weeks.
Possible side effects include pain, swelling, or itching at the injection site. These usually appear with the first injections and can be managed by cooling the area or taking an antihistamine tablet.
Food Allergies

Not every unpleasant reaction after eating is an allergy. Adverse reactions to food have many different causes, and a true allergy is only one of them.
Types of Reactions to Food
-
Psychosomatic Reaction
An aversion to food can bring on nausea or vomiting. Eating disorders fall into this category as well. - Toxic Reaction
Caused by contamination of the food (for example by moulds). Prevention rests on proper storage. - Infectious Reaction
Develops after eating spoiled food. It presents as diarrhoea and vomiting. Treatment is mainly about adequate rehydration. - Food Intolerance
Not driven by the immune system; for example, due to enzyme deficiency.- Histamine intolerance: flushing, runny nose, digestive trouble.
- Lactose intolerance: bloating, diarrhoea, dependent on the amount of milk consumed.
- True Food Allergy
The only reaction driven by the immune system. Diagnosis includes a clinical history, skin and laboratory tests, and where appropriate, elimination and oral food challenge testing.
Food allergy affects roughly 6 to 8% of children and about 3% of adults. Most discomfort after eating is therefore not allergic in origin.
If symptoms appear, the first step is usually a visit to your general practitioner, who will advise on the next step or refer you to a specialist.
Allergen Immunotherapy
Allergen immunotherapy (also called desensitisation or allergen vaccination) is the only treatment that addresses the cause of an allergy directly, because it works on the mechanism of the unwanted allergic reaction and tips it back toward a healthy response. It involves giving the patient gradually increasing, regular doses of the allergen that causes their problems (for example pollen or house dust mite), with the goal of inducing tolerance so that the body becomes accustomed to the allergen. Treatment usually lasts three to five years. The allergen is given either as a sublingual solution or tablet placed under the tongue, or by injection.
Drug Allergies

Diagnosing a drug allergy rests above all on a thorough clinical history. The doctor wants to know the name and form of the medicine, why it was taken, how soon symptoms appeared, how they progressed, how severe they were, and what treatment was given and with what result.
Other medicines being taken at the time and overall health (for example infection, asthma, chronic urticaria) are also important. In cases of repeated reactions, the patient fills in a structured questionnaire.
Which Tests Are Used
- Laboratory Tests
Used in early reactions (within an hour). A positive result can confirm an allergy; a negative result does not rule one out. - Skin Tests
The basic method for confirming an allergy (for example to penicillin). Antihistamines have to be stopped before the test. Results are read at several time points. - Drug Provocation Testing
The most reliable way to rule out an allergy or to confirm tolerance of a medicine. Used only when the risk of a reaction is low.
The aim of the workup is to estimate the likelihood of a true allergy and to identify which medicines can be taken safely.
Common “False” Drug Allergies
Penicillin Antibiotics
Penicillin allergy is often overstated. In reality, fewer than 10% of patients with this label are truly allergic.An incorrect label leads to the use of less suitable antibiotics, with greater strain on the body and a higher risk of resistance. When the risk is low, the allergy can be safely ruled out by testing.
Local Anaesthetics
A genuine allergy is very rare. More often the reaction is to stress or pain (for instance weakness or palpitations). The allergy can be checked by testing, and a safe alternative chosen if needed.
“Iodine Allergy”
There is no allergy to iodine itself, but to specific substances that contain it.
It is important to distinguish between:
- reactions to iodine-based disinfectants
- reactions to iodinated contrast media
Modern contrast media trigger reactions less often. In most cases the risk can be assessed and reduced through appropriate prevention.
Thank you for reaching out to us.
One of our team members will be in touch shortly through your preferred method of communication.
Thank you for reaching out to us.
One of our team members will be in touch shortly through your preferred method of communication.
We Will Get Back to You Within a Few Days
The contact form is intended for new patients only. Existing patients are kindly asked to communicate by e-mail at alergologie@gennet.cz.
We greatly appreciate your interest in making an appointment at our allergy and clinical immunology outpatient clinic. At present, our capacity is significantly limited, especially for patients with allergies.
Once capacity becomes available, we will be pleased to welcome you.
A referral from a general practitioner or another referring physician is required for the examination.
Thank you for your understanding.
The team of doctors and nurses
Gennet Allergy and Clinical Immunology Outpatient Clinic
